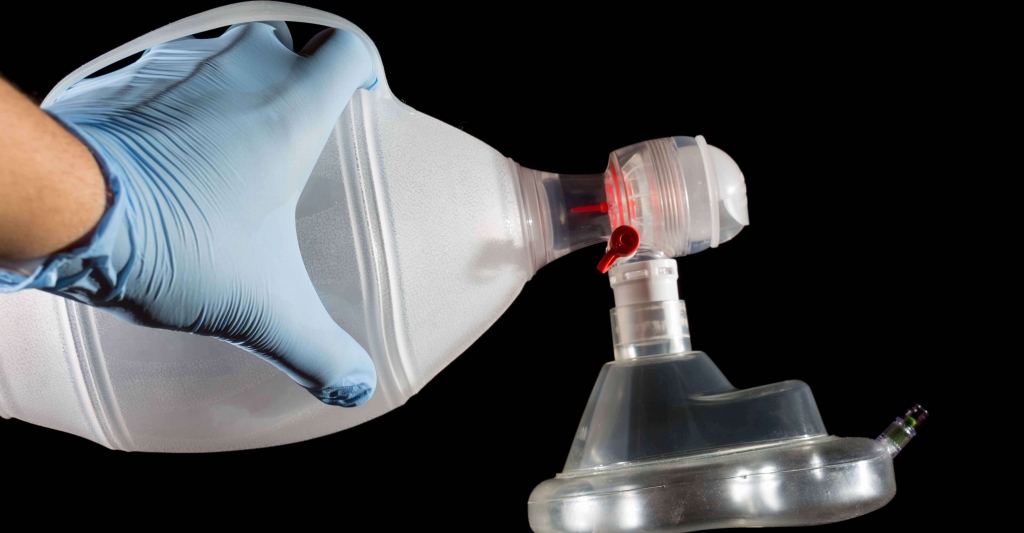
During our initial EMT training, we were all taught how to perform one- and two-person bag-valve mask ventilation.
But what happened when you started performing simulated respiratory and cardiac arrests in the lab setting? What about if you were lucky enough to witness an arrest in the clinical setting? What about every respiratory and cardiac arrest patient you have attempted to resuscitate since obtaining your EMS certification? I have been in EMS since 1992. I can count on one hand the number of times I performed or asked a team to perform two-person bag mask ventilation — zero, zip, nada.
The argument has always been that we do not have the resources available to commit two people to ventilating the patient — one person holding the mask with an E-C grip and the other squeezing the bag until he or she sees the chest rise.
But is that really true? No. I know some of you reading this are going to say, “But Rich, I work in the rural environment and we don’t have enough manpower!” Guess what? You do have enough manpower.
If you are working for a volunteer department and you are the only person on the scene, you clearly have an argument that you don’t have the manpower. If you work for a paid rural service, you do. I’ll circle back around to this point, but first, why do we need to worry about it?
AHA bag mask ventilation guidelines
In 2010, the American Heart Association introduced the two-person bag mask ventilation guideline. It was reintroduced in 2015 because the majority of care providers ignored it.
To be honest, I didn’t even know it was a guideline until I was researching ventilation while building all new 24- and 48-hour lectures on the topic last year.
The guideline clearly did not get the attention that the AHA hoped it would in 2010, and even now it still isn’t getting much notice. When I discuss the subject during the associated airway lectures, students consistently say they have never heard the recommendation and I get a lot of push back for the reasons I stated above.
We all know there are people who are extremely difficult to intubate, especially in the pre-hospital setting where we don’t always have the advanced tools and medications to facilitate the intubation.
It is estimated about 1% of the population cannot be ventilated by one person. One percent? That’s not too bad! Or is it?
According to the United States Census Bureau, as of July 1, 2018, there were about 327,167,434 people in the U.S. As EMS professionals, we’re not generally good with math, but that 1% who can’t be ventilated comes out 3,270,000+ people.
According to the World Population Clock, there are 7.7 billion people on the planet. So, 1% of the world population is 77,000,000 people. We are literally encountering these people every single day. We are doing our patients a great disservice by not following the AHA guideline.
Here are some issues that negatively affect our ability to ventilate a patient using the one-person method:
- Angioedema
- Down Syndrome patients have some significant facial and head abnormalities that need to be considered
- Edentulous patients (partial or complete loss of teeth)
- Facial hair
- Facial trauma
- Lack of padding – infants and small children should have a folded towel under their shoulders and older kids and adults should have padding under the occiput
- Macroglossia
- Obesity
How we can implement this live-saving change
Let’s circle back to the most recent reiteration of the two-person bag mask ventilation guideline. Initial training programs are being targeted. Think back to your EMT lab training. Was there any reason you could not have asked your “partners” to perform two-person bag mask ventilation? No.
There are numerous EMT students standing around trying to be wallflowers to avoid being sucked into the scenario. If we train our students to perform a given task in the lab setting, we increase the likelihood that the task will be performed in the pre-hospital environment. It’s all they know!
We also have to address this concept in our continuing medical education (CME) programs. EMS people do not like change. We hate it. But this must change.
If we incorporate this concept into our CME programs, the new EMTs and paramedics won’t receive perplexed looks when we perform the task together. We can force the change to occur.
It has to be in everything we do, from biannual skills assessments and CPR re-certifications to ACLS, PALS and trauma re-certifications.
Grab a partner and get to it
I live in Las Vegas, and when we respond to a critical event like a cardiac arrest, there are eight people on the scene — two in the ambulance, two on the fire rescue and four on the fire engine.
Is there any reason we can’t perform two-person bag-valve mask ventilation in my community? No, especially considering we should not be transporting patients in this situation unless we obtain a return of spontaneous circulation.
What about those of you who work for paid rural departments where you only have two people on scene?
There is definitely going to be a time when it is not possible to perform two-person bag mask ventilation during the initial treatment of the patient. One person is performing CPR while the other is applying the heart monitor or AED, and your advanced care provider is going to be initiating an IV to administer medications.
But after completing these essential tasks, you can switch to two-person bag mask ventilation. One provider should be holding the mask while the other is performing compression and can move to squeeze the bag after the 30 or 15 compressions, depending on if you are treating an adult or a child, respectively.
Dedicating one person to hold the mask with two hands is also going to improve passive ventilation.
No more excuses! Two-person bag mask ventilation is essential. Just do it!