Chest wall trauma is the third most common blunt injury in the “unintentional injury” category, behind head injuries and extremity injuries.
These injuries are on the verge of moving into the second most common blunt injury and account for up to 60% of all trauma-related deaths.
Chest wall injuries can cause death within a few minutes because both the respiratory and circulatory systems are involved. Trauma to the respiratory system results in direct injuries to the lungs or airways, and the impaired respiration is rapidly fatal.
Intrathoracic pressure increases because air and/or blood accumulates around the lungs reducing the patient’s tidal volume. The increase in pressure reduces the lungs’ ability to expand the increase in intrathoracic pressure on the heart, which decreases the patient’s preload and prevents contractions.
Bleeding within the chest cavity can also impair circulation because of a decrease in venous return that impairs cardiac filling and increased intrathoracic pressure. Blunt trauma can also injure the heart resulting in heart failure and damage to the heart valves.
Let’s review some different types of chest wall trauma.
Rib Injuries/Flail Chest
Injury to the chest wall also can impair respirations and range from a rib fracture to a flail chest. The pain caused by these injuries associated with breathing results in a decrease in tidal volume.
A flail chest, defined as an acute chest injury in which two or more ribs become detached from the rest of the ribcage, is commonly difficult to recognize in the prehospital setting.
As per the latest Centers for Disease Control and Prevention’s (CDC) Guidelines for Field Triage of Injured Patients, a study completed by the Israel National Trauma Registry stated that a flail chest was only identified in 262 out of 118,211 trauma patients, 0.002%, and in 262 of 11,966 chest injuries, 0.02%.
Because these injuries are so difficult to identify, it is recommended we assess for chest wall instability and deformity because this more accurately identifies what EMS providers are trained to assess for in the prehospital setting.
This change ensures that patients with blunt trauma to the chest and multiple rib fractures will be transported to an appropriate facility.
As much as we love to splint orthopedic injuries, rib injuries should not be splinted. The splint will further impair inspiration resulting in atelectasis, which can lead to hypoxemia, the development of pneumonia, or both.
Tension Pneumothorax
A tension pneumothorax occurs when air becomes trapped within the thoracic cavity. This type of injury is more commonly seen with penetrating trauma to the chest wall, also known as a sucking chest wound.
The U.S. military states that a tension pneumothorax is the second leading cause of death in a combat environment. As intrathoracic pressure continues to increase, pressure is applied to the great vessels, trachea, and the uninjured lung.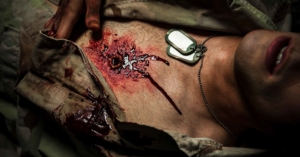
The patient will then present with jugular venous distension, diminished to absent breath sounds, hyperresonance when the chest is percussed and tracheal deviation. Tracheal deviation is commonly referred to as a late sign because we are taught to visualize the area.
By the time we see tracheal deviation the patient is in cardiac arrest because of a lack of blood flow to the heart.
Do not wait until you visualize tracheal deviation to act and palpate the trachea. Place your index and ring finger on either side of the sternal notch and locate the trachea with your middle finger. You can feel the tracheal deviation long before you can see it.
The treatment for a tension pneumothorax first requires you to seal the chest wall injury with your hand, then with an occlusive dressing. If the patient develops symptoms of a tension pneumothorax, you should first attempt to burp the occlusive dressing to relieve the pressure.
If symptoms do not resolve, you will need to obtain a 3.25-inch 14-gauge needle. Then, locate with second or third intercostal space, mid-clavicular line and insert the needle. Then remove the needle and leave the catheter.
You should hear a rush of air, and the patient’s symptoms will improve. Keep in mind that when you are measuring for the midclavicular line that the clavicle goes all the way to the distal edge of the shoulder. Also, do not stop at the proximal shoulder because you will be too close to the mediastinum.
Hemothorax
A hemothorax occurs when blood accumulates within the pleura, compressing and displacing the lung. A massive hemothorax occurs when there is more than 1,500 milliliter of blood within the pleural space.
Signs and symptoms of a hemothorax include flat neck veins with signs of:
- Hypovolemia
- Ventilatory insufficiency
- Dull percussion
- Anxiety
- Chest pain
- Dyspnea if the patient is conscious
Treatment of a hemothorax includes supportive care, high-flow oxygen, two large-bore intravenous (IV) lines, and transport.
Keep in mind, a needle decompression of a hemothorax is an absolute contraindication. By keeping the chest wall intact, we are hoping to slow bleeding as the pressure increases within the chest cavity. By decompressing the chest, the blood has an avenue to escape which decreases the intrathoracic pressure.
Cardiac Tamponade
A cardiac tamponade occurs when fluid accumulates in the pericardial sac is compressing the heart and decreasing cardiac output. There are normally 10 to 50 milliliters of fluid within the pericardium, it only takes an accumulation of 100 milliliters of fluid to stop the heart from contracting.
The patient will present with Beck’s triad, muffled heart tones, hypotension, and jugular venous distension. You also may see electrical alternans on the cardiac monitor.
Electrical alternans occurs when consecutive, normally conducted QRS complexes alternate in height. This variation in QRS height is produced by the heart swinging backward and forward within a large fluid-filled pericardium.
Prehospital management of this patient consists of regular reassessment and management of the patient’s airway, breathing, and circulation (ABCs), administer oxygen, start an IV and transport.
